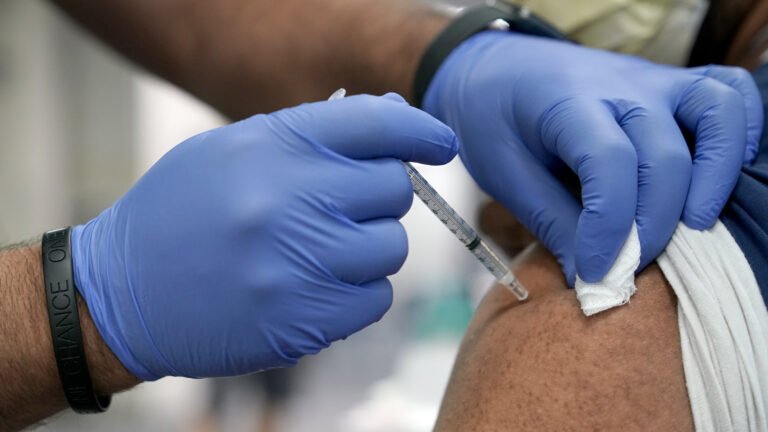
The same week that Rochelle Walensky, the director of the Centers for Disease Control and Prevention, gave the green light to booster shots for Pfizer vaccine recipients over age 65, the World Health Organization reported that only 2.2% of people in the world’s low-income countries had received even one dose of a Covid vaccine.
That means millions of Americans will receive a third vaccine dose while billions around the world have not had their first.
That stark contrast of U.S. haves and global have-nots prompted one of my clinic patients to ask me, “Is it immoral for me to get a booster?”
My response is in my new article at Boston Globe’s STAT news: https://www.statnews.com/2021/10/15/feeling-guilty-about-getting-covid-booster-shot-do-this/

![[ M U R M U R S ]](http://images.squarespace-cdn.com/content/v1/51efa33ce4b09afa04cb2a66/1376911411704-LDY4UEIH1WRGPUXTMLJU/Logo.jpg?format=1500w)